Camille Finn, RD, Director of Nutrition, Health & Wellbeing
Conventional wisdom suggests that families worry most about whether aging parents are eating well. The Fork in the Road: A Study by Age of Majority for Restaura challenges that assumption. When caregivers were asked to name their single biggest concern related to overall nutrition and eating, 44% identified hydration — ranking it ahead of getting enough fresh, nutritious food, eating unhealthy foods, and getting enough calories.
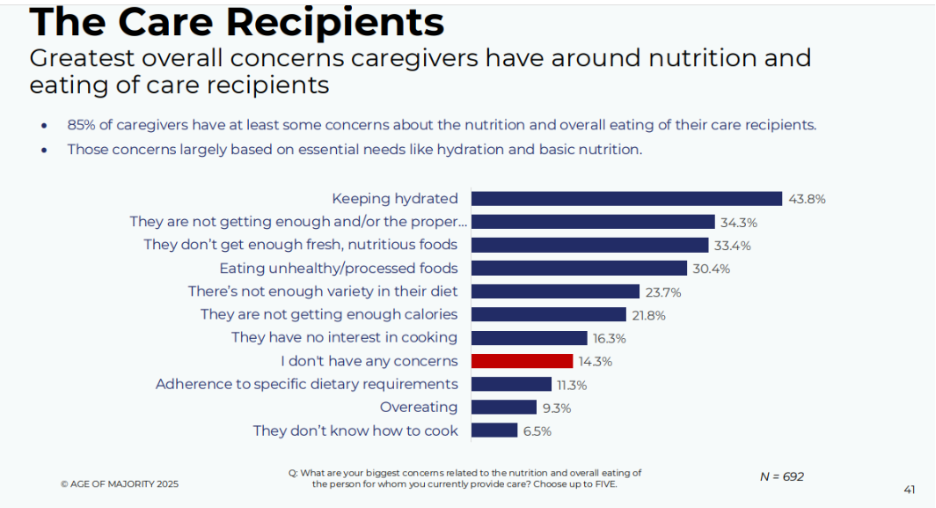
That finding is striking. It signals that families aren’t only thinking about what their parents are eating; they’re worried about whether something more basic is quietly being missed. Hydration, often treated as secondary or assumed, has become the most immediate nutrition concern in the eyes of those closest to aging adults.
This awareness may surprise some operators. But it reflects a deeper shift in how families understand aging: less focused on individual meals or nutrients, and more focused on daily consistency, function, and prevention.
What the Research Confirms: A Clinical Leadership Perspective
As a Registered Dietitian, I’ve seen hydration issues show up again and again, rarely as the primary diagnosis, but frequently as a contributing factor. It’s there in the background of falls, infections, fatigue, and hospital readmissions. And yet, hydration is still most often addressed reactively, after something has already gone wrong.
The Fork in the Road findings align with what clinicians and operators see every day. Research shows that even mild dehydration – as little as a 1–2% loss of body water—can impair cognitive function, concentration, and mood in older adults. Dehydration has also been linked to increased risk of falls, urinary tract infections, constipation, and hospitalizations.
What clinical experience reveals is that dehydration is rarely about refusal or noncompliance. More often, it reflects systems and environments that weren’t designed with hydration in mind.
Are beverages readily available throughout the day?
Are they appealing and varied?
Are there natural prompts built into daily routines?
Is hydration integrated into dining and hospitality – or left to reminders alone?
When hydration is treated as everyone’s responsibility, rather than no one’s, outcomes improve.
Why Hydration Becomes More Complex with Age
From a clinical perspective, hydration becomes more challenging as we age for several reasons. Thirst sensation diminishes over time, meaning older adults may not feel thirsty even when their bodies need fluids. Kidney function changes, muscle mass decreases (reducing total body water), and many commonly prescribed medications – such as diuretics – increase fluid loss.
The result is that dehydration in older adults is often subtle and cumulative rather than dramatic or acute. Fatigue, mild confusion, dizziness, or changes in appetite can all be early signs. Too often, hydration is addressed only after it contributes to a larger issue, such as a fall, infection, or hospitalization.
One of the challenges with hydration is that it’s frequently oversimplified. Telling someone to “drink more water” doesn’t account for preferences, routines, physical limitations, or enjoyment.
Hydration comes from many sources: water-rich foods like soups, fruits, and vegetables; warm beverages such as herbal teas; and flavored waters that offer variety without added sugar. Temperature, texture, timing, and accessibility all matter.
Just as importantly, hydration should feel like a natural part of the dining experience versus a separate task or clinical reminder.
A Generational Shift and a Quiet Opportunity for Senior Living
Today’s family caregivers, many of whom are Gen X or Millennials, are thinking differently about aging than generations before them. They are asking deeper questions about freshness, quality, function, and prevention. Hydration fits squarely into this shift. It’s no longer an afterthought; it’s part of how families define good care.
At the same time, hydration represents one of the greatest “quiet wins” in senior health and wellbeing. It doesn’t require new technology or complex clinical protocols. Small, consistent practices embedded into daily routines and dining experiences can have a meaningful impact on energy, cognition, comfort, and overall vitality.
Hydration deserves the same intentionality as food quality and nutrition strategy. Across senior living communities, some of the most effective hydration strategies are also the simplest:
– Offering beverages consistently throughout the day, not just at meals
– Incorporating soups, smoothies, and other high-water-content foods into menus
– Making hydration stations visible, accessible, and inviting
– Providing variety in temperature and flavor to encourage intake
– Training team members across dining and care to view hydration as part of the resident experience
These approaches reinforce hydration as a shared priority and align closely with what families are telling us matters. The opportunity now is to meet that awareness with thoughtful, person-centered approaches that support aging well. Sometimes the most powerful interventions are also the least flashy. Hydration is one of them.

About Camille Finn, RD, Director of Nutrition, Health & Wellbeing
Camille is an experienced Registered Dietitian with a Bachelor’s degree from Cornell University and a Master’s from the Tufts Friedman School, specializing in corporate wellness and foodservice management. She combines a passion for culinary arts with a dedication to sustainability, viewing nutrition-centered prevention as a vital key to long-term wellness.
References
Armstrong, L. E., et al. (2012). Mild dehydration affects mood in healthy young women. Journal of Nutrition, 142(2), 382–388.
National Institute on Aging. Dehydration and older adults. U.S. Department of Health and Human Services.
Popkin, B. M., et al. (2010). Water, hydration, and health. Nutrition Reviews, 68(8), 439–458.

